The hidden cost of fragmented training, workflows, and patient materials
Mar 31, 2026
The hidden cost of fragmented training, workflows, and patient materials
Fragmentation rarely looks dramatic at first.
It usually shows up as smaller problems that seem manageable on their own: onboarding takes longer than it should, teams explain the same process differently, patient materials do not fully match what happens in practice, and staff rely on memory or workarounds to keep things moving.
Individually, those issues may not look like a systems problem. Together, they create something harder to ignore: inconsistency in how care is delivered.
What fragmentation actually looks like
In many organizations, training, workflows, patient-facing materials, and documentation supports were built at different times, for different needs, by different people. Some pieces may be strong on their own. The problem is that they were never designed to function as one connected system.
That disconnect shows up when:
-
staff are trained one way, but workflows push them another
-
patient materials set expectations that do not fully match real encounters
-
updates happen in one part of the system while the rest stays outdated
-
teams rely on verbal clarification instead of shared structure
At that point, the issue is no longer whether the materials exist. The issue is whether they work together.
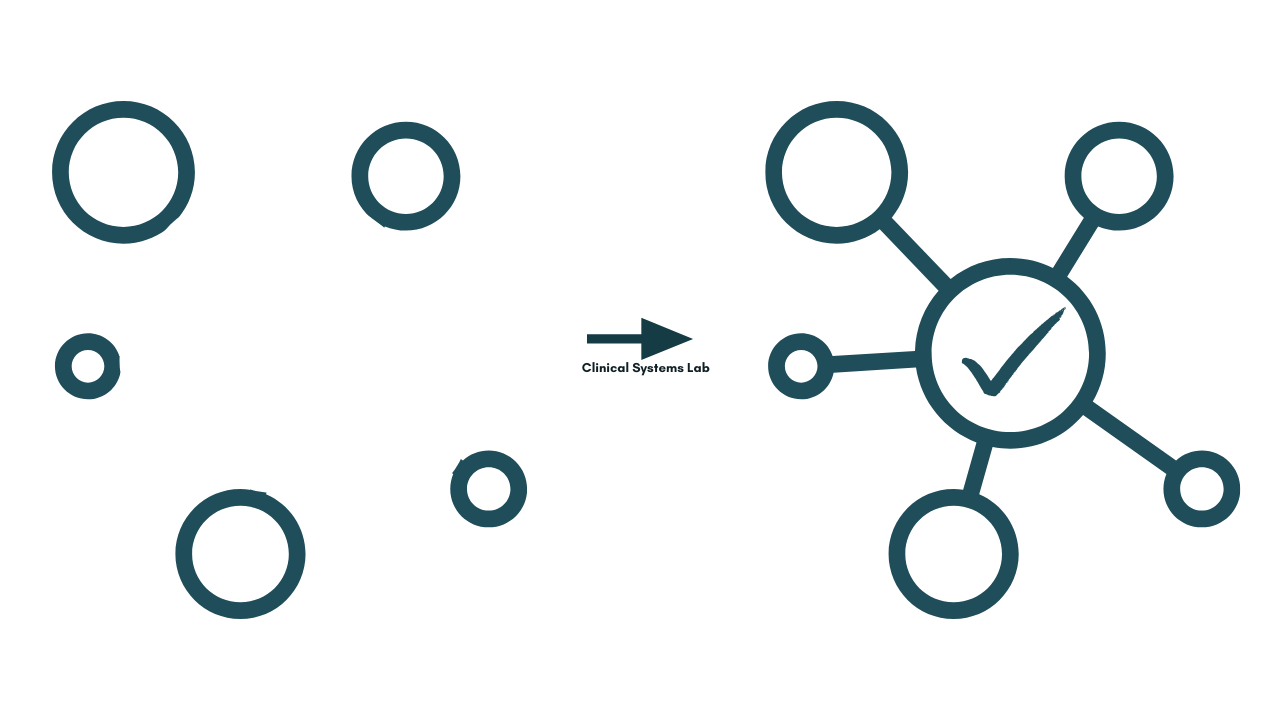 The cost is higher than it looks
The cost is higher than it looks
Fragmentation creates operational drag.
New staff take longer to get oriented because they are not just learning the work. They are learning which version of the process is current, what people actually do, and where the unofficial fixes live.
Teams become less consistent because each person starts bridging the gaps differently. Patients get a more variable experience because communication, expectations, and follow-through are not fully aligned. What feels survivable in a small team becomes harder to manage across roles, locations, and growing programs.
The cost is not just clutter. It is variation.
Why one isolated fix rarely works
This is where teams often lose time.
A visible pain point appears, so one piece gets updated: a handout, a workflow, a training deck, a script. That may help at one touchpoint. But if the surrounding system is still disconnected, the broader problem remains.
A new asset can improve one part of the experience without changing the structure around it.
That is why isolated fixes often underperform. The issue is not always the quality of the new piece. The issue is that it is being dropped into the same fragmented environment that created the problem in the first place.
What a connected system changes
A connected system makes it easier for training, workflows, and patient-facing materials to reinforce the same model of care.
That improves more than organization. It improves clarity.
Teams spend less time guessing which process is current. Onboarding gets easier. Updates are easier to apply consistently. Patient communication becomes more aligned across the care experience. Delivery depends less on memory and individual workarounds.
That is usually the real goal.
Final takeaway
The hidden cost of fragmentation is not just inefficiency. It is inconsistency in how care is prepared, communicated, and delivered.
And that is rarely solved by one more isolated update.
If your training, workflows, and patient-facing materials have evolved separately over time, the next step may not be another standalone fix. It may be a clearer system.
Get new insights from Clinical Systems Lab
Subscribe for occasional insights on workflows, implementation, and patient-facing tools.
We hate SPAM. We will never sell your information, for any reason.

